- Home
- Respiratory Rehabilitation
- Sleep Breathing Disorders
- Product Center
- Professional Zone
- About Us
- Contact Us

Breathing rehabilitation is a rehabilitation process that improves respiratory function, enhances exercise tolerance, and optimizes quality of life through comprehensive intervention methods for individuals with respiratory dysfunction or related diseases. It integrates respiratory training, physical exercise, nutritional guidance, psychological support, and other aspects, and is applicable to conditions such as chronic obstructive pulmonary disease, asthma, interstitial lung disease, and postoperative respiratory function decline.
Normal respiratory function is the foundation for the operation of all body systems, and breathing rehabilitation can help gradually restore impaired respiratory function, reduce the distress caused by dyspnea, allow patients to re-adapt to daily activities, and return to a healthy life rhythm. If you or someone around you experiences difficulty breathing, shortness of breath after activity, or similar issues, consider learning about breathing rehabilitation to support respiratory health.
Contact UsImpaired respiratory function is like an "invisible枷锁" (shackle) on the body. Simple daily activities may be limited due to shortness of breath and wheezing. Over time, this can lead to a vicious cycle of "shortness of breath - reduced activity - decreased physical fitness - more shortness of breath." Approximately 650 million people worldwide suffer from chronic respiratory diseases, and 80% of the 100 million COPD patients require breathing rehabilitation.
Breathing rehabilitation can break this cycle: it strengthens respiratory muscle strength, improves endurance, reduces shortness of breath, helps patients easily complete daily activities, improves psychological issues such as anxiety, enhances self-care ability, reduces the risk of hospitalization for acute exacerbations, and improves quality of life.
A chronic airway inflammatory disease characterized by persistent airflow limitation, manifesting as long-term cough, sputum production, shortness of breath, worsening symptoms after activity, and possible respiratory failure in advanced stages. It is the third leading cause of death worldwide, with an irreversible course but progression can be slowed through intervention.
Causes:
Smoking (main trigger), harmful substances damaging the airways;
Long-term inhalation of air pollution, occupational dust (such as coal dust, asbestos);
Recurrent lung infections, damaging airway structure;
A small number are related to genetic factors (such as α₁-antitrypsin deficiency).

A chronic airway inflammatory disease characterized by recurrent episodes of wheezing, shortness of breath, chest tightness, or cough, often triggered by exposure to allergens, cold air, with symptoms worsening at night or early morning. It can be effectively controlled through standardized treatment but is prone to recurrence.
Causes:
Genetic factors, family history of allergies or asthma significantly increases risk;
Environmental factors: inhalation of allergens such as pollen, dust mites, animal dander, or irritants like air pollution, smoke, perfume;
Immune abnormalities: excessive reaction of the body to allergens, leading to airway mucosal edema, smooth muscle spasm, and airway narrowing.

A pulmonary infectious disease mainly affecting alveoli and lung interstitium, manifesting as fever, cough, sputum production (purulent or bloody sputum), rapid breathing, chest tightness, and in severe cases, difficulty breathing, hypoxemia, or even shock. It can be classified as lobar pneumonia, bronchopneumonia, etc. based on the infection site.
Causes:
Infectious factors: pathogens such as bacteria, viruses, mycoplasma, chlamydia invading the lungs, causing inflammation;
Decreased immunity: elderly, children, patients with chronic diseases, or those taking immunosuppressants for a long time are susceptible to pathogens;
Environmental factors: polluted air, poor ventilation, or contact with respiratory tract infection patients increase the risk of cross-infection.
Respiratory function limitation caused by abnormal thoracic structure (such as sternum, rib, or spinal deformities), manifesting as difficulty breathing after activity, chest tightness, decreased endurance, and in severe cases, recurrent lung infections, respiratory failure, and possibly delayed growth and development in children.
Causes:
Congenital factors: such as funnel chest, pigeon chest, congenital scoliosis, mostly due to genetic or embryonic development abnormalities leading to reduced thoracic volume and compression of lung tissue;
Acquired factors: long-term poor posture in adolescents, spinal tuberculosis, chest trauma, or surgical sequelae, leading to changes in thoracic structure and gradually restricting lung expansion.

A disease characterized mainly by pulmonary interstitial fibrosis, manifesting as progressive difficulty breathing, dry cough, fatigue, and in severe cases, hypoxemia due to oxygen exchange disorders. The course is mostly chronic progressive, with some types having a poor prognosis.
Causes:
Occupational and environmental exposure: long-term inhalation of dust (such as silica, asbestos), metal powder (such as aluminum, iron), or contact with chemicals (such as formaldehyde);
Autoimmune diseases: such as rheumatoid arthritis, lupus erythematosus, which can involve the lung interstitium and cause inflammation;
Drugs and infections: side effects of some chemotherapy drugs, antibiotics (such as amiodarone), or viral infections (such as COVID-19) may induce it.

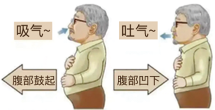
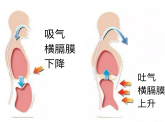
By consciously using diaphragm contraction, it increases tidal volume, reduces respiratory rate, and relieves shortness of breath.
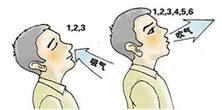
When exhaling, purse the lips like whistling to delay airway collapse, increase lung gas expulsion, and improve gas exchange.
Using resistance trainers for inspiratory or expiratory resistance exercises to strengthen respiratory muscles such as the diaphragm and intercostal muscles.

Such as walking, cycling, swimming, etc., gradually increasing intensity based on the patient's physical condition to improve cardiopulmonary endurance.

Training for limbs and core muscles to enhance exercise capacity and reduce respiratory burden during activities.

Developing dietary plans based on the patient's weight and condition, such as适当增加蛋白质摄入 for COPD patients to avoid malnutrition leading to decreased respiratory muscle strength.

Through psychological counseling, relaxation training, etc., to alleviate patients' fear and anxiety about difficulty breathing and enhance rehabilitation confidence.

Teaching patients to correctly use inhalers, oxygen therapy equipment, etc., master emergency handling methods during acute exacerbations, and improve self-management abilities.
If you have two or more of the following conditions, you may need to undergo a breathing rehabilitation assessment:
Significant shortness of breath during daily activities (such as climbing 1 flight of stairs, brisk walking)
Frequent cough and sputum production affecting quality of life
Significant reduction in activity level due to respiratory problems (e.g., previously able to walk 1 km, now only 200 meters)
Hospitalization for respiratory-related diseases once or more in the past six months
Chronic lung diseases (such as COPD, asthma) with poor symptom control

Deep Breathing Trainer
One breath, one vibration, clear breathing anytime

Deep Breathing Trainer Advanced Version
Protect every breath of yours

Pulmonary Function Tester
Portable respiratory health testing

Portable Oxygen Concentrator
Easy travel, free breathing

Respiratory Detection and Training Device
Precise detection, professional diagnosis

High-Flow Respiratory Humidification Therapy Device
Intelligent temperature and humidity control for more comfortable treatment